Treatments & Services
Gynecologic Cancer Treatments | Robotic Surgery, Chemotherapy & more
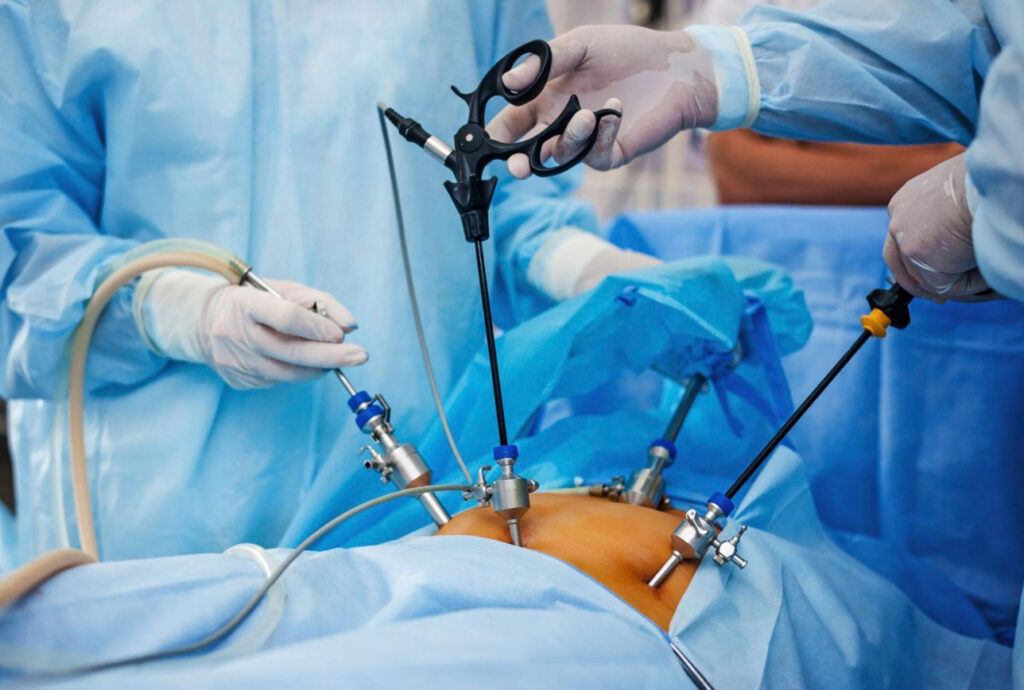
Laparoscopic Surgery in Gynecological Oncology
Laparoscopy has become a key minimally invasive approach in the management of gynecologic cancers. It offers diagnostic, staging, and therapeutic benefits with improved recovery and reduced morbidity, without compromising oncologic outcomes.
1. Advantages of Laparoscopy in Onco-Gynecology
- Minimal invasiveness → smaller incisions, less pain
- Reduced blood loss
- Shorter hospital stay and faster recovery
- Lower risk of wound complications (especially in obese or diabetic patients)
- Better visualization with magnified view of pelvic anatomy
- Quicker postoperative start of adjuvant therapy
2. Major Oncologic Applications
a) Endometrial Cancer
- Laparoscopic extra fascial total hysterectomy + BSO
- Pelvic and para-aortic lymphadenectomy
- Sentinel lymph node mapping with ICG
- Comparable survival outcomes to open surgery (supported by LAP2 trial)
- Particularly beneficial in obese patients
b) Cervical Cancer
- Early-stage cancers: laparoscopic radical hysterectomy + lymphadenectomy
- Allows nerve-sparing technique
- However, after LACC trial, conventional laparoscopy shows inferior survival vs. open in early cervical cancer.
Current approach: Avoid laparoscopic radical hysterectomy unless:
- No uterine manipulator
- Closed vaginal cuff technique
- Tumor <2 cm
- Done in experienced high-volume centers
(Ongoing studies evaluating safe modifications)
c) Ovarian Cancer
- Staging of apparent early-stage tumors
- Peritoneal biopsies, omentectomy, lymphadenectomy
- Evaluation of operability in advanced cases (diagnostic laparoscopy, Fagotti score)
- Selected secondary cytoreductive surgery
Not preferred for bulky stage III/IV disease requiring aggressive debulking.
3. Specific Procedures Possible Laparoscopically
- Hysterectomy (simple or radical)
- Pelvic lymphadenectomy
- Para-aortic lymphadenectomy (up to renal vessels)
- Omentectomy
- Pelvic exenteration in selected cases
- Retroperitoneal exploration
- Trachelectomy (highly selected early cervical cancer)
4. Oncologic Safety
- Multiple studies show equivalent disease-free and overall survival in endometrial and ovarian cancers when oncologic principles are respected.
- For cervical cancer, modifications are required to maintain oncologic safety (as above).
5. Limitations
- Steep learning curve for complex onco-procedures
- Limited access in resource-poor settings
- Restricted ergonomics compared to robotics
- Difficult in very obese patients or dense adhesions
- Risk of tumor spill if not handled carefully
6. Contraindications
- Hemodynamically unstable patients
- Very bulky cervical tumors (>4 cm) for minimally invasive radical surgery
- Disseminated disease requiring extensive upper abdominal debulking
- Severe cardiopulmonary compromise (can’t tolerate pneumoperitoneum)
7. Role in Sentinel Lymph Node Mapping
- Use of Indocyanine Green (ICG) enhances lymphatic visualization
- Best established for endometrial and cervical cancers
- Reduces need for full lymphadenectomy → less lymphedema and morbidity
8. Postoperative Outcomes
- Faster bowel recovery
- Lower analgesic requirement
- Early mobilization and reduced DVT risk
- Earlier discharge and return to normal activities
Need a consultation? Contact us to know our availability and contact details.

Dr Richa Bansal
Dr. Richa Bansal MBBS, MS (Obstetrician and Gynecologist), DNB, MCh Gynecological Oncology (Tata Memorial Hospital, Mumbai) is a Sr. Consultant Gynecological Onco Surgeon, Laparoscopic & Robotic Surgeon
What we say?
What our patients say?
Image Gallery